Neonatal Phototherapy
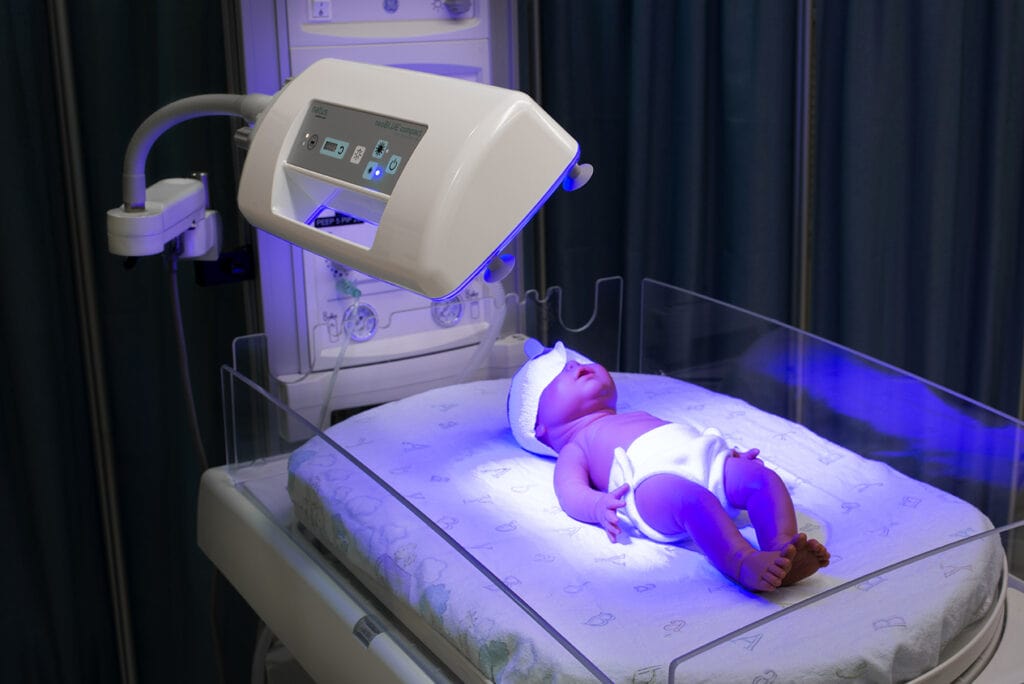
Neonatologist in Nagpur - Dr. Shilpa Hazare
Neonatal Phototherapy:
The use of visible light to treat severe jaundice in newborns is known as phototherapy. Clinically observable jaundice affects around 60% of term neonates and 85% of preterm babies. It usually occurs on day 3, peaks on days 5-7, and resolves in 14 days for term babies and 21 days for preterm babies. Dr. Shilpa Hazare is a Neonatologist in Nagpur, Consultant Pediatric Intensivist, Pulmonologist, and Bronchoscopist who provides Neonatal Phototherapy.
Phototherapy is used to avoid the neurotoxic consequences of excessive unconjugated bilirubin levels in the blood. Phototherapy is a safe and effective way to lessen the need for exchange transfusions in newborns by lowering or avoiding the increase of serum unconjugated bilirubin levels.
It’s occasionally used to treat infant jaundice by reducing bilirubin levels in your baby’s blood through a photo-oxidation process.
The bilirubin undergoes photo-oxidation, which adds oxygen to it and allows it to dissolve efficiently in water. This makes it easier for your baby’s liver to break down and remove bilirubin in their blood.
Phototherapy is classified into two types.
- Conventional Phototherapy – Conventional Phototherapy is placing your kid in front of a halogen or fluorescent bulb with their eyes closed.
- Fibreoptic Phototherapy – Your baby rests on a blanket with fibreoptic cables; the light goes through the cables and shines on your baby’s back.
Management:
Nutrition:
Unless clinically contra-indicated owing to other pathologies, breastfed newborns who require phototherapy should continue to breastfeed; the neonate’s sucking, attachment, and mother’s milk production should all be monitored. If a newborn is reaching the point of needing an exchange transfusion, the infant should not be taken out of phototherapy to feed because this is a medical emergency. If feeding is considered safe, all feeds should be administered via a bottle or NGT.
Neonatal who are getting EBM or neonatal formula via enteral feeding should continue to do so. When a newborn is getting phototherapy, the total fluid intake (TFI) for a 24-hour period may need to be raised by at least 10% to allow for insensible fluid loss, although this should be guided by hydration status and electrolyte monitoring.
Parenteral feeding and IV fluids should be continued as prescribed, with a 10% increase to allow for insensible fluid loss.
Phototherapy:
- Start phototherapy after the TSB/SBR exceeds the prescribed reference range for the neonate’s gestation/weight and the presence of risk factors.
- Under phototherapy, neonates should be breastfed nude except for a diaper, and they will need to be nursed in an Isolette to maintain a neutral temperature environment. To maximize skin exposure, the diaper may need to be removed and a urine bag used in extreme instances.
- Positon phototherapy units should be kept at a distance of no more than 30.5cm from the patient. Phototherapy device may be placed as near to the patient as 15cm.
- Expose as much of the skin’s surface to the phototherapy light as feasible. Dress the infant merely in a diaper and their protective eye coverings to maximize skin exposure.
- Use suitable opaque eye coverings.
- During newborn care or feeding, make sure the eye coverings are removed every 4-6 hours for eye care. Observe for any signs of discharge, infection, or injury, and record any changes.
- For pregnant and postnatal age, daily fluid requirements should be assessed and tailored.
- Follow a fluid balance chart to the letter.
- If the bilirubin level is high, breastfeeding may need to be reduced to 20 minutes to reduce the amount of time spent out of the lights.
- Monitor vital signs and temperature at least every four hours, and more frequently if necessary.
- To avoid peroxidation, cover lipid lines with light-resistant, reflective tape.
- When collecting blood for TSB/SBR levels, make sure the phototherapy device is switched off since both conjugated and unconjugated bilirubin are photo-oxidized when exposed to white or ultraviolet light.
- Keep an eye out for symptoms of possible adverse effects.
What are the Potential Complications?
- Lactose intolerance is just temporary
- Infants with conjugated hyperbilirubinemia are ‘bronzed.’
- Damage to the retina
- Overheating – keep an eye on the temperature of the newborn.
- Increased peripheral blood flow and diarrhea cause water loss (if present)
- Irritable bowel syndrome (IBS) causes diarrhea.
- Ileus (preterm infants)
What are the Risk Factors in Neonatal Phototherapy?
- Instrumental birth causes cephalhaematoma, bruising, and trauma.
- Incompatibility with ABO
- Incompatibility with Rh
- Breastfeeding insufficient
- Mothers who tested positive for antibodies
- G6PD deficiency runs in the family
- A sibling who was previously afflicted
- Meconium passage is delayed.
- Prematurity
- Dehydration
Why Choose Dr. Shilpa Hazare?
Dr. Shilpa Hazare has a special interest in pulmonology and bronchoscopy. She is one of the best Neonatologist in Nagpur. She provides Neonatal Phototherapy and has 20 years of experience in this field.

Dr. Shilpa Hazare
MD (Paed), DCH, DNB Consultant Neonatologist, Pediatric Intensivist, Pulmonologist, and Bronchoscopist.
- 20 Years Of Experience
- Special Interest In Pulmonology and bronchoscopy.
- Mon-Sat | 10 AM to 5 PM
