Neonatal Intensive Care (NICU) Level III
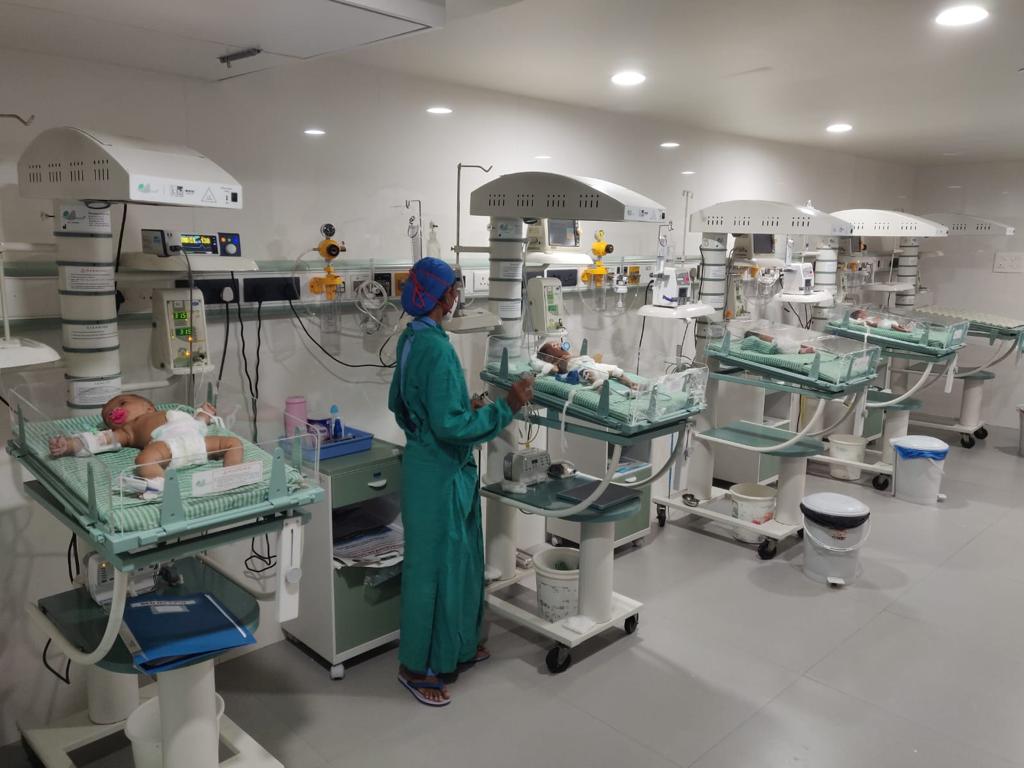
Neonatal Intensive Care Unit
The NICU is developed for ill newborns that require particular treatment, using equipment specifically built for infants and medical staff properly educated in newborn care. Babies that need to be admitted to the facility are usually admitted within the first 24 hours following their birth. Premature newborns, babies with low or extremely low birth weight, babies with congenital problems, and babies with difficulties such as meconium aspiration or respiratory infections are typically admitted to the NICU. Dr. Shilpa Hazare is working as a Senior Consultant at Getwell Hospital and Research Institue which is known as the best Neonatal Intensive Care Unit.
The Centre for Child Health includes the departments of neonatology and neonatal intensive care at Getwell Hospital and Research Institute. A highly specialized team of Neonatologists, Newborn Nurses, and Allied Health Specialists oversee a comprehensive variety of services for complicated medical and surgical neonatal disorders. They use a multidisciplinary approach to provide complete treatment to patients, enlisting the help of several different teams and departments within the hospital.
The Neonatology and Neonatal Intensive Care Unit is divided into three sections for newborns that require particular attention:
- Level III Neonatal Intensive Care Unit
- Unborn newborns are cared for in a step-down nursery.
- An place of seclusion
Neonatal Intensive Care (NICU) Level III:
Level III units must have the same care professionals as Level II facilities (pediatric hospitalists, neonatologists, and newborn nurse practitioners) and Level I facilities (pediatric hospitalists, neonatologists, and neonatal nurse practitioners) (pediatricians, family physicians, nurse practitioners, and other advanced practice registered nurses).
In addition, Level III facilities must include pediatric surgeons, pediatric medical subspecialists, pediatric anesthesiologists, and pediatric ophthalmologists on-site or through planned consulting arrangements at a closely affiliated institution.
Level III newborn intensive-care units can do the following tasks:
- Consistently provide life support
- Provide comprehensive treatment for critically sick neonates born at all gestational ages and birth weights.
- Provide immediate access to pediatric medical subspecialists, pediatric surgical experts, pediatric anesthesiologists, and pediatric ophthalmologists.
- Provide a comprehensive spectrum of respiratory assistance, including conventional and/or high-frequency breathing, as well as nitric oxide inhalation.
- Perform sophisticated imaging, including computed tomography, MRI, and echocardiography, with immediate interpretation.
There are three types of Level III NICUs.
Level III-A: is capable of
- Providing complete treatment to children delivered after 28 weeks of pregnancy and weighing more than 1000 grammes.
- Apgar scores of 3 and lower are considered critically low.
- Provide only conventional mechanical ventilation for long-term life support.
- Minor surgical procedures such as central venous catheter implantation or inguinal hernia repair are performed.
Level III B NICU: capable of providing
- Comprehensive care for extremely low birth weight newborns (/=1000g and/=28 weeks’ gestation).
- For as long as needed, advanced respiratory assistance such as high-frequency ventilation and inhaled nitric oxide
- Access to a comprehensive spectrum of paediatric medical subspecialists quickly and on-site.
- Advanced imaging, such as computed tomography, magnetic resonance imaging, and echocardiography, with immediate interpretation
- Major surgery, such as ligation of patent ductus arteriosus and repair of abdominal wall defects, necrotizing enterocolitis with bowel perforation, tracheoesophageal fistula and/or oesophagal atresia, and myelomeningocele, is performed on-site or at a nearby institution by paediatric surgical specialists and paediatric anesthesiologists.
Level III C NICU has the same capabilities as a level IIIB NICU but is situated in a facility that can offer extracorporeal membrane oxygenation and surgical correction of severe congenital heart abnormalities that necessitate cardiopulmonary bypass.
Some Risk Factors that necessitate NICU admission:
Factors affecting mothers –
- Bleeding during pregnancy is a common occurrence
- STIs (sexually transmitted infections)
- Amniotic fluid that is either too little or too much
- Membrane rupture that occurs too soon
- Exposure to drugs or alcohol
- Age ranges from 16 to 35 years
- Diabetes, hypertension, or heart disease may be present
- Pregnancies in multiples
Factors affecting delivery –
- Birth asphyxia/fetal distress
- Breech presentation, meconium-stained liquor, cord around the neck Forceps, or caesarean birth are all examples of abnormal presentation.
- Other types of birth injuries
Baby-related factors –
- Defects in the pregnancy
- Distress in the lungs (rapid breathing, grunting or apnoea)
- Infection \sSeizures
- Phototherapy is required for neonatal jaundice
- Blood transfusion is required
- Extra oxygen or monitoring, as well as IV or other drugs, may be required.
- Blood sugar levels are low
- Before 37 weeks or beyond 42 weeks, a baby is born
- Weight at birth: less than 2500 gms or more than 4 kgs
- For gestational age, this is a small baby
- In the delivery room, resuscitation is performed
